Repeat failures put the brakes on research until the pharma industry regrouped in a new, non-competitive, way.
By Pierre Meulien, IMI Director
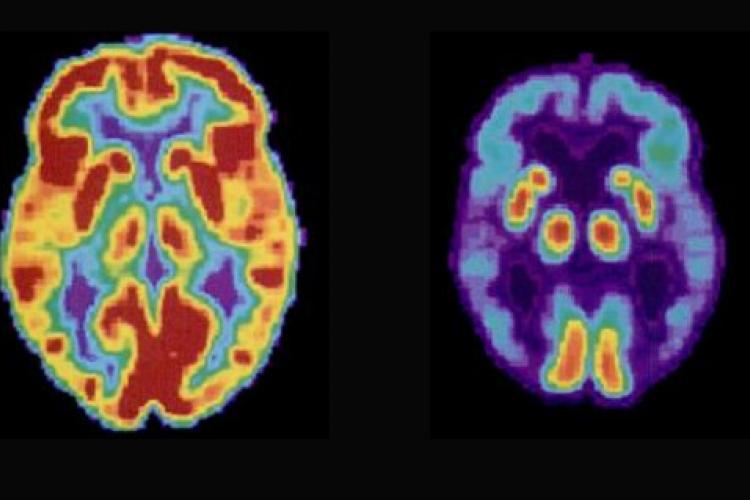
A ten-billion euro failure
Pharmaceutical companies spent years, and upwards of 10 billion euro, looking for an effective treatment for Alzheimer’s disease. And they failed. A lot of the failure happened at phase three trials, the worst-case scenario for a pharmaceutical company: a promising molecule that produces encouraging results is found to be safe, only to be revealed to be ineffective during an expensive trial with thousands of people.
It’s fair to say that this failure was due in no small part to the isolation in which these researchers were working. Alzheimer’s research is highly competitive. These companies had been working alone and in competition with each other. Their research often revolved around treatment of late-stage dementia, a treatment for which would give them access to a very lucrative market, but that is extremely difficult to treat. In recent years, there has been a collective admission of defeat and it’s only because of initiatives like IMI that the industry is having another go.
Why past research failed
Having worked in isolation, pharma companies, and academics, had not shared the reasons for the failure of clinical trials. They may have enrolled people that didn’t have Alzheimer’s at all; people who failed cognitive tests, but then turned out not to have any amyloid in their brain. Researchers from academia would publish their work in journals, but their results were often unreproducible by pharma companies.
The difference now, regrouped under a public private partnership, is that they are able to share their lessons, mistakes and data from years of unsuccessful attempts, and include other critical voices, such as patients and regulators. The contribution from patients, in particular, is not mere tokenism – they are the ones who will ultimately determine the viability of any potential new drug. IMI research is looking much more at the underlying biology rather than going after late-stage cures. We know now that there has been too much focus on the build-up of beta-amyloid in the brain that leads to the plaque, the hallmark of the disease. Beta-amyloid is the end-point, but what led to it? We need to go much further back. We now know that it can appear in the brain up to 20 years before any symptoms manifest, and that there are people with beta-amyloid who never get symptoms at all.
Video: IMI-funded researchers are going after Alzheimer's much earlier.
Hidden Alzheimer's
One of IMI’s biggest strengths is our ability to select, with laser precision, the right people for trials. There is a lot of “hidden” Alzheimer’s lurking in healthy people, and our projects MOPEAD and EPAD are trying to find it. We created a clinical research platform with several thousand people who do not have Alzheimer’s, and we’re carrying out deep phenotyping and looking for trends so that we can build profiles of people that might be susceptible to certain interventions. Researchers are also looking for molecules that can prolong the length of time between early-onset and late-stage. They are examining the underlying mechanisms of the disease, the link with inflammation (PHAGO), the role of apolipoprotein E, the most well-known genetic risk factor for Alzheimer’s (ADAPTED), and protein misfolding and the spread of disease proteins like tau (IMPRIND).
Alzheimer’s is a scientific failure, unlike AMR, another neglected area of research that IMI has taken on, which is a market failure. Both types are suited to public private partnerships because they offer companies a chance to pool what they’ve learned from years of research. Without a PPP many would be reluctant to get involved in Alzheimer’s again – indeed, some still are. We have incentivised risk-sharing for one of the most burdensome diseases and enticed companies back to the drawing board.
Read more
IMI Alzheimer's research projects
Alzheimer's researchers use AI to get access to brains
Alzheimer’s project EPAD releases first wave of data to research community
PET scans that show brain changes caused by Alzheimer’s give doctors confidence in diagnosis
